
by All Things Neonatal | May 1, 2019 | IVH
Recently the practice of keeping ELBW infants with a midline head position for the first three days of life has been recommended to reduce IVH as part of a bundle in many units. The evidence that this helps to reduce IVH has been somewhat circumstantial thus far. Studies finding that decreased sagittal sinus blood flow, increased cerebral blood volume with increased intracranial pressure all occur after head turns would theoretically increase the risk of IVH. Raising the head of the bed would help in theory with drainage of the venous blood from the head and in fact systemic oxygenation has been shown to improve with such positioning. This presumably is related to increased cardiac output from better systemic venous return.
Bringing it to the bedside
Interestingly, some of the above studies are from over thirty years ago. We now have some evidence to look at involving this practice. Kochan M et al published Elevated midline head positioning of extremely low birth weight infants: effects on cardiopulmonary function and the incidence of
periventricular-intraventricular. The study involved maintaining ELBW infants in an elevated midline head position (ELEV- supine, head of bed elevated 30 degrees, head kept in midline) versus standard head positioning (FLAT–flat supine, head turned 180 degrees every 4 h) during the first 4 days of life to see if this would decrease in the incidence of IVH. Ninety infants were randomized into both arms of the study. In terms of baseline characteristics, BW of 725g in the FLAT vs 739 in ELEV were comparable as well as GA both at 25 weeks. Two differences on the maternal side existed of 40% ELEV vs 24.4% FLAT of mothers having preeclampsia and 23.3% FLAT vs 10% ELEV having prolonged rupture of membranes both of which were statistically significant.
What did they find?
Ultrasounds were performed at entry into the study and then daily for days 1-4 and then on day 7 with abnormal scans repeated weekly. In terms of IVH the authors noted no overall difference in rate of IVH. What they did find however was a statistically significant reduction in the rate of Grade IV IVH.
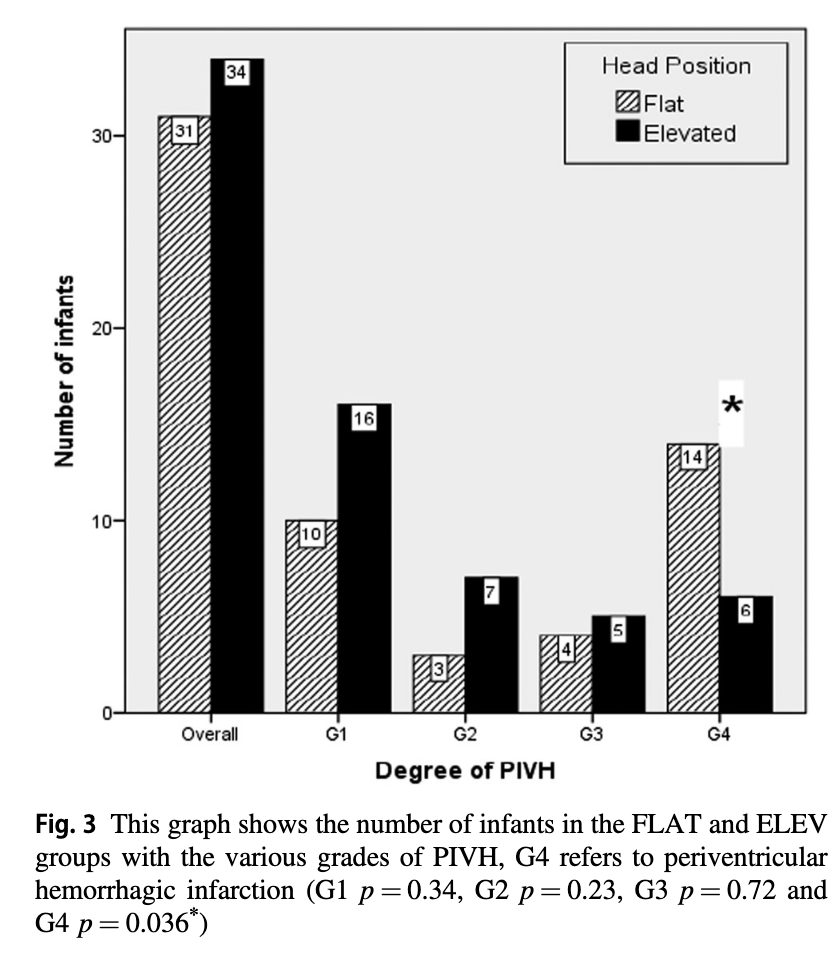
The p value for the finding of lower rates of Grade IV IVH was 0.036 so not strikingly significant but different nonetheless. Given that the venous drainage of the head is also dependent on the resistance to flow from the pressure in the thorax one can’t infer that the intervention alone is responsible for this without ensuring that that respiratory findings are similar as well. Similarly without knowing inflow of blood into the head as measured by blood pressure it is difficult to say that the reduction in IVH isn’t related to differences in blood pressure.
The authors helpfully looked at both of these things. For those infants on high frequency ventilation the mean airway pressure was higher on day one being 11.5 cm H2O (FLAT) vs 9.9 cm H2O (ELEV) neither of which are high although different. The rest of the three days were no different. For those on conventional ventilation the only difference was on day 4 where the MAP was higher for ELEV at 8 vs 7.4 cm H2O which again is fairly mild. Interestingly, as was found in other studies that oxygenation was improved with elevation of the head, the maximum FiO2 for the two groups was different on day 1 being 46% in the FLAT vs 37.5% in the ELEV.
Looking at the hemodynamic side of things there were differences in the lowest mean BP recorded on day 1 and 3 but otherwise the groups were similar.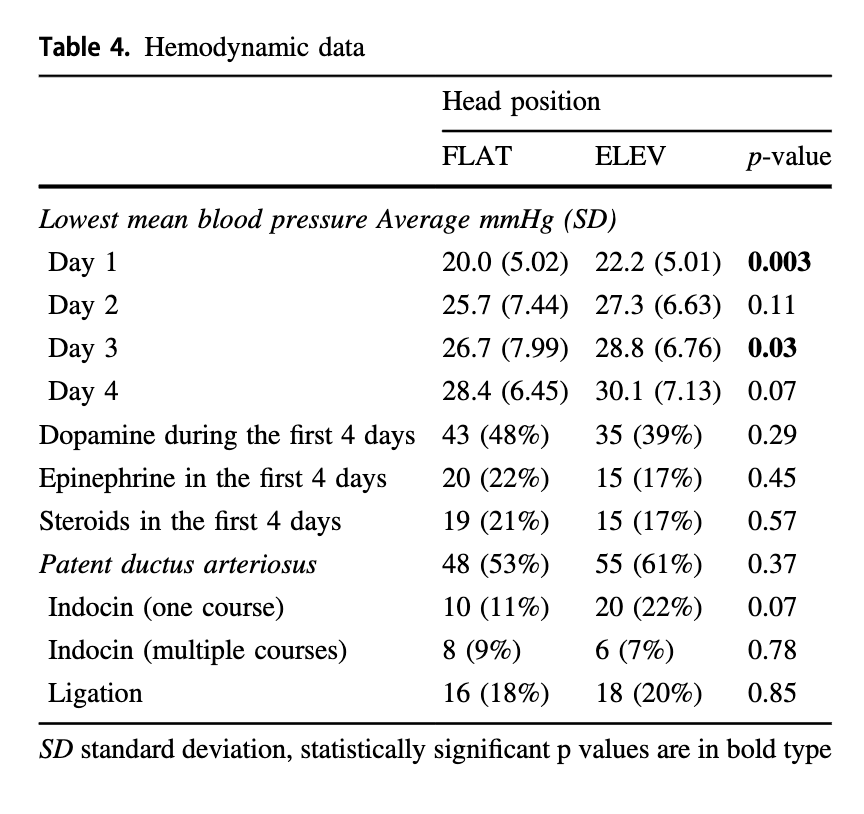 It would have been nice to see mean results during this time rather than lowest but this is what we have.
It would have been nice to see mean results during this time rather than lowest but this is what we have.
In terms of complications of preterm birth there were no differences found in rates of sepsis (important given the increase rate of prolonged rupture in the FLAT group), NEC or ROP.
Although length of stay was no different 92 vs 109 days ELEV (NS), survival to discharge was at 88% vs 76% (p=0.033) which also may explain the longer length of stay.
What Can We Learn From This
Don’t worry. I am not about to throw the results out. There are a couple observations though that need to be addressed. The first is the increased rate of preecampsia in the ELEV group. This finding could have impacted the results. We know that fetuses exposed to this condition are stressed and are often born with better lungs than their non-exposed counterparts. The endogenous increase in steroids due to this stress is attributable and may explain the better oxygenation and lower mean airway pressures needed in the ELEV group rather than improvements in flow alone from positioning. The second issue is adherence to the protocol as there were some infants in the ELEV group who were placed flat for the final 1-2 days of the study. Having said that, this would serve to dilute the effect rather than strengthen it so perhaps it makes the results more believable.
So where does this leave us? This study demonstrates improved survival and a reduction in Grade IV IVH without an overall reduction in IVH. There was nothing found to suggest that the intervention is harmful. Given the background studies demonstrating improved systemic oxygenation, reductions in ICP and cerebral blood volume the finding of reduced severe IVH seems plausible to me. This could be a practice changing study for some units who have perhaps only adopted midline positioning in the first few days of life. It will be interesting to see if this takes off but is certainly worth a good look at.

by All Things Neonatal | Dec 19, 2018 | Prematurity
Recent statements by the American Academy of Pediatric’s, NICHD, the American College of Obstetricians and Gynecologists (ACOG), the Society for Maternal-Fetal Medicine (SMFM), and recommend selective approaches to mothers presenting between 22 0/7 to 22 6/7 weeks. The decision to provide antenatal steroids is only recommended if delivery is expected after 23 weeks. Furthermore the decision to resuscitate is based on an examination of a number of factors including a shared decision with the family. In practice this leads to those centres believing this is mostly futile generally not resuscitating or offering steroids while other more optimistic hospitals having higher rates of proactive (steroids and resuscitation) rates. Then there are other centres where the standard approach is proactive such as one in Uppsala, Sweden where this approach is used almost exclusively.
What would happen then if one compared the outcome for infants born at 22 weeks between this hospital and another where a selective approach is generally offered. In this case you would have a lot of experience with resuscitating infants at 22 weeks and the other a fraction of all presenting as a few to many would receive compassionate care. This is exactly what has now happened.
A Tale of Two Cities
The University Children’s Hospital, Uppsala, Sweden has been compared retrospectively to Nationwide Children’s Hospital, Columbus, Ohio, USA (NCH) with respect to survival and outcomes for their infants born at 22 weeks. The paper by Backes CH et al entitled Outcomes following a comprehensive versus a selective approach for infants born at 22 weeks of gestation tells a very interesting story about the power of belief or faith that one can accomplish something if they set their mind to it.
The authors examined a period from 2006-2015, dividing this time into two epochs with the first being 2006-2010 to account for differing practices and resources over time. Given that Uppsala took a proactive approach to all of their 40 live born infants during this time, it provided an opportunity to look at the 72 infants who were live born in the Ohio and examine their differences. In Ohio the approach was as follows; 16 (22%) received proactive care, 18 (25%) received inconsistent care (steroids but no resuscitation), and 38 (53%) received comfort care. In other words, although the total number of infants live born in Ohio was almost double that of Uppsala, only 16 were proactively treated in Ohio compared to all 40 in Uppsala.
The differences in outcome are striking
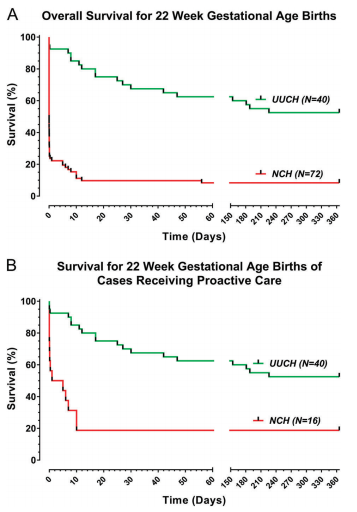
Survival in delivery room: (38/40, 95% vs 12/16, 75%; P = 0.049)
Provision of delivery room surfactant: (40/40, 100% vs 9/16, 56%; P<0.01)
Survival at 24 h (37/40, 93% vs. 9/16, 56%; P < 0.01).
Survival to 1 year (21/40, 53% vs. 3/16, 19%; P < 0.05).
Among the infants treated proactively, median age of death (17 postnatal days at range 0 h–226 days vs. 3 postnatal hours at NCH, range 0 h–10 days; P < 0.01).
All surviving infants had BPD All infants surviving to initial hospital discharge were alive at 18 months’ postnatal age.
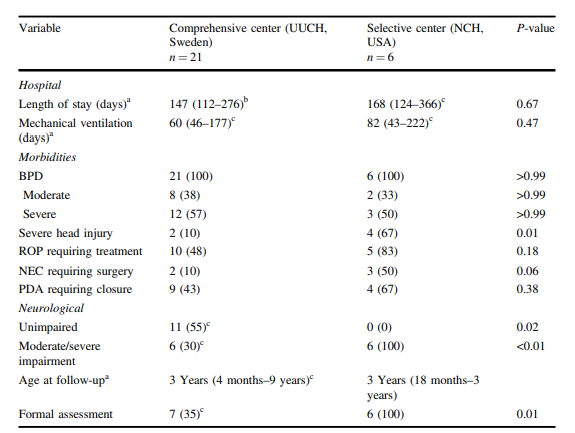
With respect to long term outcome the authors note:
“Outpatient follow-up (qualitative or non-qualitative neurodevelopmental testing) was available in 26 out of 27 infants (96%) Eleven of the 26 (42%) were unimpaired, and all unimpaired infants were in the UUCH cohort. Among the 15 infants with impairment at UUCH, 3 had mild impairment and 12 had moderate or severe impairment. All surviving infants at NCH had moderate or severe impairment.”
A word about antenatal steroids as well. In Uppsala 85% of mothers received 2 doses of antenatal steroids vs 25% in Ohio. People sometimes question whether ANS at this age are effective. It is interesting to note that 44% of babies in the Ohio group vs 3% p<0.01 received chest compressions +/- epinephrine in the delivery room. Might this explain the better state of some of these infants at birth?
The Power of Belief
When I do rounds I often remark that try as we might we can’t will babies to do better. I also commonly say however that we need to be optimistic and although I am accused of seeing the world through rose coloured glasses I think there is an important lesson to be learned from this study. This comparison is really a contrast between a system that believes they can do a good thing for these families by actively promoting a proactive approach vs a system in which I imagine a reluctant approach exists even for those infants where a proactive plan is enacted. One sign of this might be that in Sweden 100% of these deliveries had a Neonatologist present vs 75% in the US. It could be due to other factors such as ability of the Neo to get in within time of the delivery however rather than a sign they didn’t feel they were needed due to futility.
There is evidence as well that the aggressiveness of the proactive approach also differs between the two sites based on a couple observations. The first is the rate of surfactant provision in the delivery room which was 100% in Sweden but only 56% in the US. The other thing of note is the time of death for those who did not survive. The median time of death in the US was 3 hours vs 17 days in Uppsala. What does this tell us about the approaches? I would imagine (although the numbers are small) that the teams in the US were much more likely to lose hope (or faith) and withdraw early while the other centre possibility motivated by their past successes pushed forward.
Remarkably, although one might think that the teams in Uppsala were simply creating significantly impaired survivors, 42% of the survivors were unimpaired from a developmental standpoint in follow-up. All surviving infants though from Ohio had moderate to severe impairment.
What this story may also really be about is practice. The reality is that the team in Sweden had over twice the exposure to such infants over time. Although the number presenting at this GA was higher, the ones that actually were resuscitated and given steroids was less than half. One cannot take away though that Uppsala in the end demonstrated that a proactive approach is definitely not futile. Not only can these children survive but almost half will be developmentally intact.
We must acknowledge as well though that since this is a retrospective study there may be factors that may have affected the results. As the saying goes “Individual results may vary”. Are the teams the same in both centres in terms of number of Neonatologists? Are there more residents caring for these infants vs fellows? Are the resources the same? What about proximity of the Neonatologist to the hospital? There are other factors such as cohesiveness of the team and communication between team members that may be influencing the results.
In the end though, this is a story of a team that believed it could and did. Perhaps seeing the world through rose coloured glasses is not such a bad thing in the end.
by All Things Neonatal | Jun 4, 2015 | Neonatology, Prematurity, Vaccination
Ask any health care professional how our tinyest babies fare after an immunization and they will tell you “not well”. In fact the belief is so pervasive that we go out of our way to find excuses to delay immunizations. I have heard myself uttering such comments as “today is not a good day” or “let’s wait until there is greater respiratory stability” or simply “they are too sick”. Perhaps this tendency develops because we are shaped by our past experiences and if we have had a baby get intubated who was on CPAP after an immunization, we subconsciously say to ourselves “that won’t happen again”.
By no means am I writing an anti-vaccination piece but rather exploring our behaviours and trying to come up with a means of changing them. Adverse Events After Routine Immunization of ELBW Infants was published on this very topic this week and with nearly 14000 infants from 23 – 28 weeks included who received their first 2 month immunization, it certainly caught my attention!
The table indicates the risks of certain adverse events in the 3 days preceding the immunization to the 3 days afterwards. 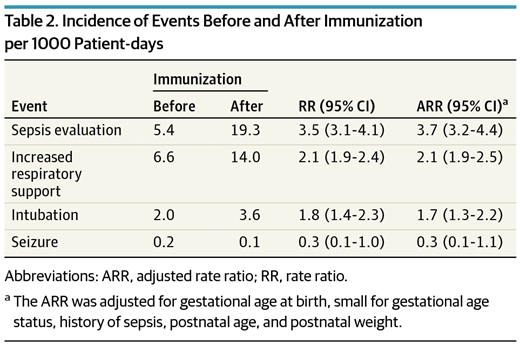 What you will note is that the evaluations for sepsis increased 4X, Respiratory support and intubation almost 2X, with no difference in seizures. It is important to note that the definitions for sepsis were based on two blood cultures being drawn rather than fever alone. Curiously with respect to sepsis there was an increase in the number of positive cultures as well from 2.1 to 3.8% in the evaluations that were done before and after. It is worth pointing out though that I can find no analysis of those results to determine if they were statistically different so at most it is an “interesting” finding.
What you will note is that the evaluations for sepsis increased 4X, Respiratory support and intubation almost 2X, with no difference in seizures. It is important to note that the definitions for sepsis were based on two blood cultures being drawn rather than fever alone. Curiously with respect to sepsis there was an increase in the number of positive cultures as well from 2.1 to 3.8% in the evaluations that were done before and after. It is worth pointing out though that I can find no analysis of those results to determine if they were statistically different so at most it is an “interesting” finding.
The figures below demonstrate the rate of the same adverse events before time zero and then afterwards for the same duration as in the table.
What you notice aside from the rise in adverse events is a sharp decline in the rate of adverse events just prior to the immunization and then a sharp rise after it is given. 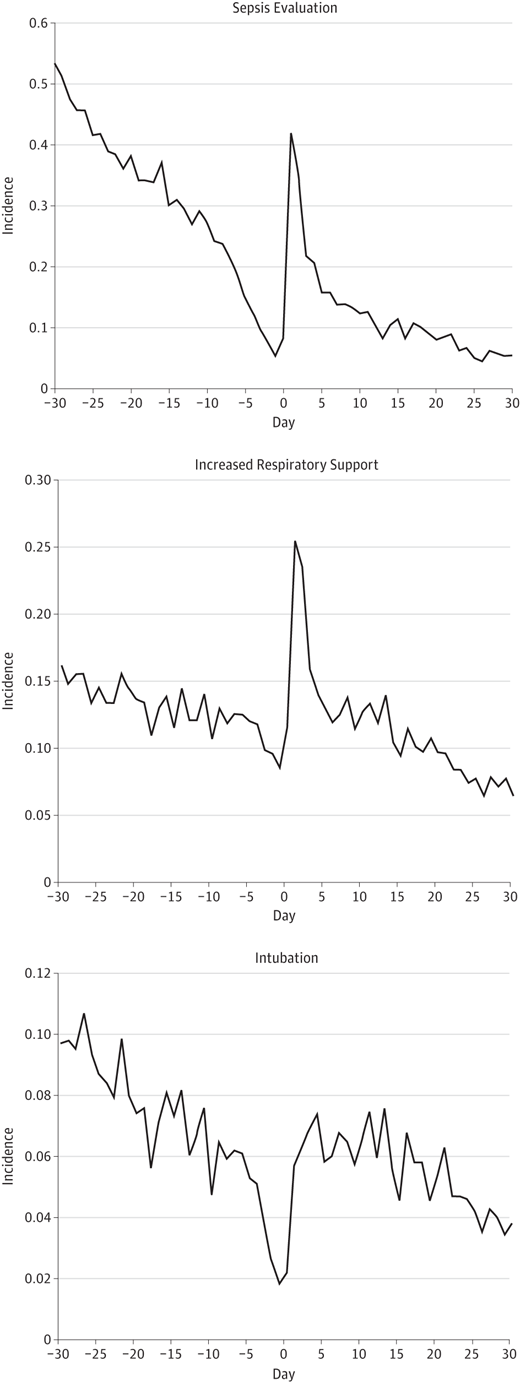 The steep decline just prior to immunization is known as the Healthy Vaccinee Effect. That is to say that we may see a higher rate of complications simply due to the fact that we wait for kids to be at their healthiest and when they have only had one or two days without apnea or are off their antibiotics that is when we choose to give the vaccine as we believe they can now “handle it”. What we have created is a special sample of patients that actually does not reflect the whole population. What I mean by this is that the response of all patients to their vaccines in this age group might be quite different with no increases in any adverse events if we paid no attention to our preconceived notions that the infant in our care is “too sick” to get their immunization. When we only immunize those kids that are at their best, the likelihood of them deteriorating is higher than when they were “worse”.
The steep decline just prior to immunization is known as the Healthy Vaccinee Effect. That is to say that we may see a higher rate of complications simply due to the fact that we wait for kids to be at their healthiest and when they have only had one or two days without apnea or are off their antibiotics that is when we choose to give the vaccine as we believe they can now “handle it”. What we have created is a special sample of patients that actually does not reflect the whole population. What I mean by this is that the response of all patients to their vaccines in this age group might be quite different with no increases in any adverse events if we paid no attention to our preconceived notions that the infant in our care is “too sick” to get their immunization. When we only immunize those kids that are at their best, the likelihood of them deteriorating is higher than when they were “worse”.
We know from previous literature that ELBW infants have higher rates of apnea and need for respiratory support after their vaccines. If we gave them an immunization when they were on CPAP or a higher dose of caffeine would we notice the impact as much? By waiting till they have weaned off CPAP or outgrown their dose of caffeine we are setting ourselves up for a setback.
Similarly perhaps the optimal time to give the vaccine is when they are actually on an antibiotic for a sepsis evaluation or have had a CRP for one reason or another in the preceding 24 hours. Would a mild fever after the vaccine trigger the same response to do a septic workup or would you take comfort in knowing your patient was already on antibiotics or had no signs of inflammation prior to the vaccine?
In summary I question if I have had it all wrong. I am not saying to give a vaccine to a patient who is on high frequency ventilation and inotropes due to septic shock but rather when they are recovering and off the inotropes but still ventilated what is the harm? They are already intubated, and covered with antibiotics. Seems to me to be the perfect conditions to prevent me from either escalating their respiratory support or doing a septic workup. They are already covered!


 It would have been nice to see mean results during this time rather than lowest but this is what we have.
It would have been nice to see mean results during this time rather than lowest but this is what we have.




 What you will note is that the evaluations for sepsis increased 4X, Respiratory support and intubation almost 2X, with no difference in seizures. It is important to note that the definitions for sepsis were based on two blood cultures being drawn rather than fever alone. Curiously with respect to sepsis there was an increase in the number of positive cultures as well from 2.1 to 3.8% in the evaluations that were done before and after. It is worth pointing out though that I can find no analysis of those results to determine if they were statistically different so at most it is an “interesting” finding.
What you will note is that the evaluations for sepsis increased 4X, Respiratory support and intubation almost 2X, with no difference in seizures. It is important to note that the definitions for sepsis were based on two blood cultures being drawn rather than fever alone. Curiously with respect to sepsis there was an increase in the number of positive cultures as well from 2.1 to 3.8% in the evaluations that were done before and after. It is worth pointing out though that I can find no analysis of those results to determine if they were statistically different so at most it is an “interesting” finding. The steep decline just prior to immunization is known as the Healthy Vaccinee Effect. That is to say that we may see a higher rate of complications simply due to the fact that we wait for kids to be at their healthiest and when they have only had one or two days without apnea or are off their antibiotics that is when we choose to give the vaccine as we believe they can now “handle it”. What we have created is a special sample of patients that actually does not reflect the whole population. What I mean by this is that the response of all patients to their vaccines in this age group might be quite different with no increases in any adverse events if we paid no attention to our preconceived notions that the infant in our care is “too sick” to get their immunization. When we only immunize those kids that are at their best, the likelihood of them deteriorating is higher than when they were “worse”.
The steep decline just prior to immunization is known as the Healthy Vaccinee Effect. That is to say that we may see a higher rate of complications simply due to the fact that we wait for kids to be at their healthiest and when they have only had one or two days without apnea or are off their antibiotics that is when we choose to give the vaccine as we believe they can now “handle it”. What we have created is a special sample of patients that actually does not reflect the whole population. What I mean by this is that the response of all patients to their vaccines in this age group might be quite different with no increases in any adverse events if we paid no attention to our preconceived notions that the infant in our care is “too sick” to get their immunization. When we only immunize those kids that are at their best, the likelihood of them deteriorating is higher than when they were “worse”.