In 2018 where do we stand on this question? Upcoming retrospective trials and work by EPIQ-4 may help to resolve this issue. In the meantime what does the existing evidence say?
The decision to extubate an extremely low birthweight infant is one of the most common sources of disagreement and anxiety in the NICU. As a resident, I recall an unwritten rule that “no baby under 750g will have a trial of extubation as they will most certainly fail”. As time went on however, studies suggested that not only is this a false statement but also that the duration of intubation was directly correlated with risk of BPD. As Danan described, for infants less than a 1000g, delaying extubation when they had reached minimal settings did not result in lower rates of BPD. Moreover 60 – 70% of infants who have such extubation attempts are not reintubated within a week, so it is possible to have success.
The detractors however express concern about the 30-40% who do require reintubation and worry that harm will be caused by such acts. Frequent concerns are voiced with respect to potential trauma to the airway leading to subglottic stenosis; potentially increasing the risk of BPD and finally the belief that attempts are futile so why put parents through the stress in the midst of perceived near certain failure. The problem with these perceptions however is that they are mostly the culmination of confirmation bias. Patients that have multiple failed extubations are remembered especially when they develop significant complications, while the ones who extubate successfully are quickly forgotten. This is not intentional in any way but simply a human tendency to follow the pattern of “the squeaky wheel getting the grease”. The preemies who do poorly are front and centre as they take up a great deal of our time & attention while the ones who do very well while celebrated, are not as easily remembered for the success they demonstrated when extubated.
Being someone who believes in extubating as soon as possible though I was surprised several months ago to find a paucity of data demonstrating that there was in fact support for the practice in terms of better outcomes being associated with early extubation. While small studies certainly pointed in that direction the real question was about to be answered in the study that follows.
Is it better to fail multiple times or be intubated once for the duration of ventilation.
This is the central question that I believe has been answered as good as it will ever be by EA Jensen et al in JAMA this past month “Effects of Multiple Ventilation Courses and Duration of Mechanical Ventilation on Respiratory Outcomes in Extremely Low-Birth-Weight Infants.” This retrospective review included 3343 infants below 1000g and examined the primary outcome of BPD and secondary outcomes of death, continued supplemental oxygen use at the time of discharge, and tracheostomy among survivors. As you might expect, regardless of whether one compared duration of ventilation or number of reintubations, variables such as need for surfactant, postnatal dexamethasone, PDA treatment and NEC became more common as exposure to either outcome increased. 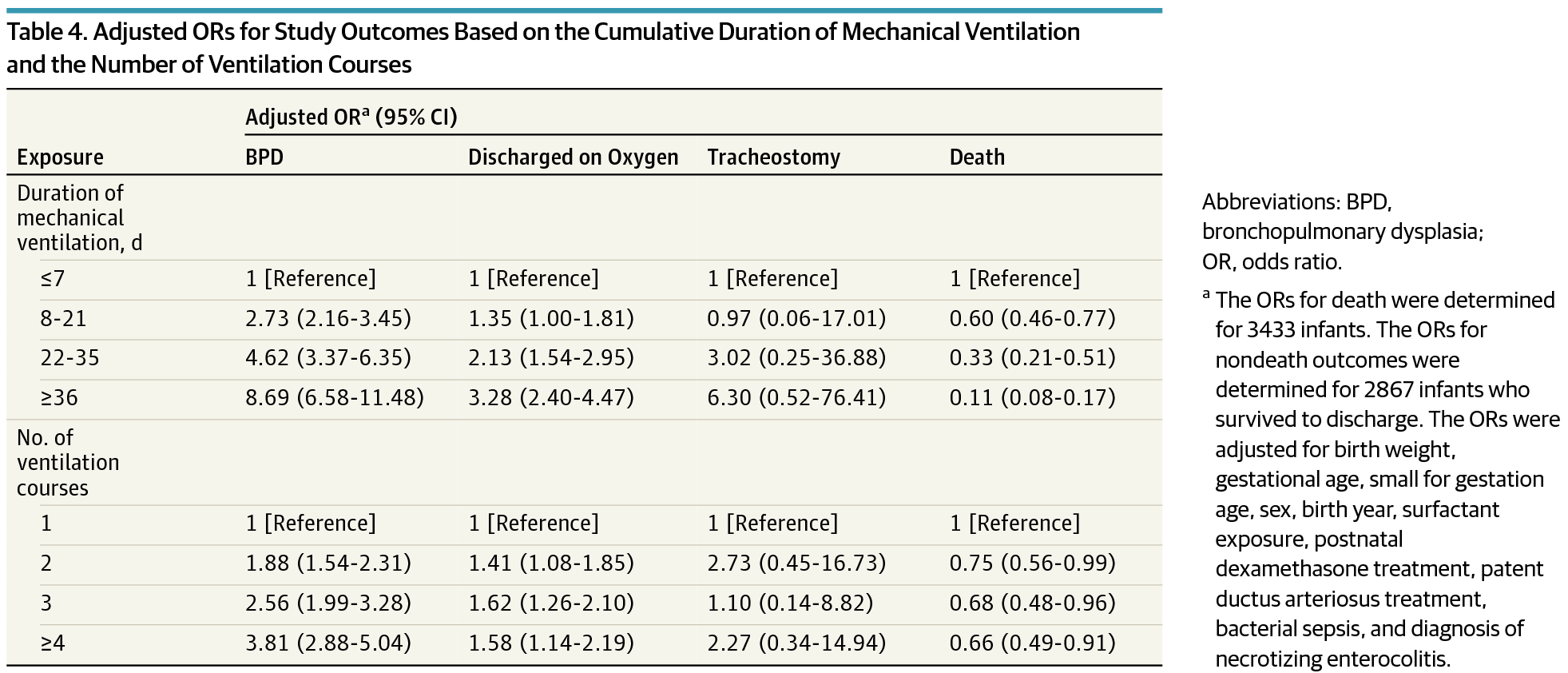 When a logistic regression model was applied though it became evident that the odds ratio for BPD increased to a much greater degree with increasing duration of ventilation than the number of attempts.
When a logistic regression model was applied though it became evident that the odds ratio for BPD increased to a much greater degree with increasing duration of ventilation than the number of attempts.
To quote the authors:
“After adjustment for the cumulative duration of mechanical ventilation, a greater number of ventilation courses was not associated with an increase in the risk-adjusted odds of supplemental oxygen use at discharge. The number of ventilation courses remained associated with increased risk of BPD only among infants exposed to 4 or more courses.”
The Needs of The Many Outweigh The Needs of The Few
In other words, for an infant to have an increased risk of BPD they would need to have failed extubation four or more times! It is not easy to predict with certainty who these children will be but if we take these findings as accurate (since I believe we will not see an RCT of this magnitude anytime soon) is it ethical to keep a child intubated due to the belief that they might fail? On the contrary, how can we not try when failure is not associated with adverse outcome? In fact none of the secondary outcomes were found to be increased either. Importantly, there was no difference in the need for a tracheostomy in this population which may serve as a proxy for lack significant airway injury from multiple intubations. The goal of this post is to provide all of us who care for these preemies with the reassurance that if they fail extubation, once, twice and even three times that is still a good thing. For the ones that fail more than that, if only we had a crystal ball we might have spared them that risk but given that we live in a world without this ability, we owe it to our patients to try. Moreover, we owe it to the parents of these children to educate them that failure can still be a good thing.
May I never have a near 100% success at extubating my patients on the first try. If I truly care for them I will embrace my failures and know that I have done the right thing.

Amazing, I am from Grand Forks, ND. We are a small unit, but we do practice early extubation. It is great so far. We underestimate these little ones.
Love hearing from our neighbours directly to the south of us!
With our two 27 week 650g preemies who are now 4 months corrected, one of them has no breathing difficulties and one does. Each of them had over 4 failed attempts, one of them had 8. This was very scary because she had a PDA ligation which didn’t appear to help, and each time she was extubated she would have a lung collapse or she would just tire herself out and stop breathing which lead to chest compressions a few times, very scary. In the end, she managed to breath with siPap and not tire herself out, but then she was 3lbs. She did have subglotic stenosis and still visits the ENT as they pulled away some granulation. We are relieved that she never had to have a tracheostomy, she is just on low oxygen at home and an NG tube for feeds. We were always upset and stressed when the NICU attempted to extubated too soon after a failed attempt, but all in all, they did deserve to try. It doesn’t always work for all preemies, but it does for some.
Thank you for sharing your experience. You are right that what determines best practice does not necessarily mean everyone will have the same experience but it is worth trying
In your opinion is it okay to keep trying? I feel the hospital we are at wants to try after the 1st or 2nd fail for a trach.
That would be pretty quick for the hospital I work at. I would think that many places would wait until several more fails before considering that
Hello! I am enjoying your blog very much. I am a neonatal nurse practitioner with 22 years experience. I was trained by physicians and NPs who were always eager for extubation trials on VLBW babies. I’m glad I learned from folks like this. And just as you say in this post, my wisest physician mentor always said, “We only remember the bad ones.” So true that the failures color everyone’s judgment. Interestingly, I am working as a locum now, and I am in a unit where they think I’m a bit nuts for pushing to extubate everyone!
Keep up the advocacy for what is best for these little ones. Glad you are getting something positive out of the posts!
My baby was born at 25 weeks. Just yesterday they attempted to extubate her again for the 4th time and they had ENT check her airways for any abnormalities. ENT didn’t find any other than swelling around the epiglottis area – trachea and bronchi are normal and no edema. Last night (on the same date as the planned extubation), my baby self-extubated by pulling the tube out with her own hands but they have to re-intubate as she was having very labored breathing and retraction. If with the tube, she is breathing at room air (21% O2) and saturating in the high 90s to 100%. So that’s why the doctors think she’s ready for extubation. But why can’t she breathe when they extubate her? They still couldn’t seem to figure out why. I’m at a loss since all her numbers were good but when they remove the tube, she couldn’t do it. Do you have any idea what could be causing her to have labored breathing after extubation? They now diagnose her with BPD as she is 36 weeks corrected age. She’s been on the ventilator for more than 10 weeks now. Hope you could share some thoughts on this matter.
Anne these questions are always difficult without seeing the whole picture. Certainly babies with BPD can have quite laboured breathing due to poorly compliant lungs. She could also be apneic and need higher doses of caffeine to stay off the ventilator. Alternatively, a course of steroids might help reduce swelling in the epiglottis area allowing for easier breathing
I’m hoping my baby does not fail his second extubation.