Our ability to breathe regularly is something most of us take for granted. We owe this function to a tiny area in the brain located in the medulla oblongata.
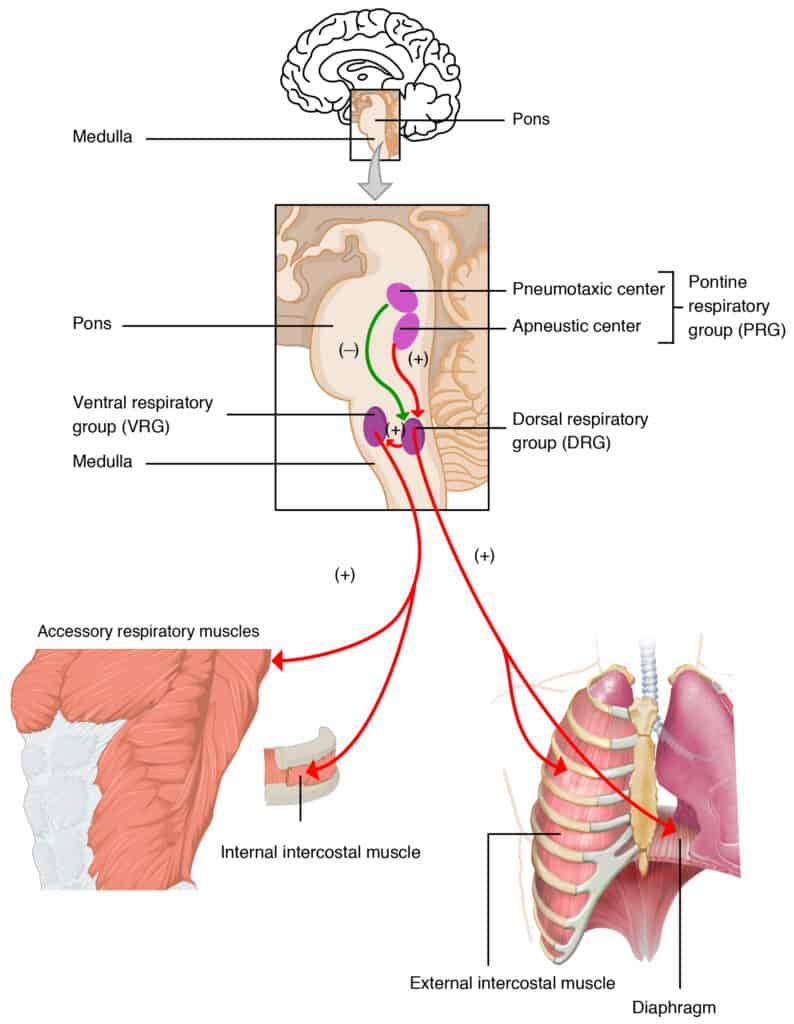
This area of the brain sends signals via nerves to the lung telling it to breathe in and out on a regular basis. For a preterm infant or even term baby this means there should be about 40-60 breaths per minute. Preterm infants are at risk for these events due to being neurologically premature but also due to a difference in the responsiveness of such infants to carbon dioxide levels in the bloodstream. In term infants and throughout life we are very responsive to higher levels of carbon dioxide. We like to keep it pretty tightly controlled which is why if you hold your breath and your carbon dioxide levels rise you feel like you need to take a breath. In preterm infants this response is blunted.
Pauses in breathing are called apnea and when they occur in a preterm infant they are known as apnea of prematurity. These are usually defined as stoppage of breathing for 20 seconds or longer or if shorter there is bradycardia (<100 heart beats per minute), cyanosis (bluish color to the skin), or pallor. They are so common under 37 weeks that I consider them a normal part of the preterm journey. You can see how common it is in the figure below. We also know that they are far more common as gestational age decreases so that a 24 week gestation preterm infant will be far more prone to apnea than the 35 week counterpart.
Parents often wonder if these drops in oxygen or heart rate are harmful. If the events are called spontaneous it means that your infant recovers quickly from these events without anyone stimulating your baby and so they are brief. We tend not to worry about these types of events as they brain is not likely to be affected. When events are happening more than a few times a day and require your nurse to either stimulate your infant or require support with a bag and mask to help your baby breathe this is where we become more concerned. Even then the presence of bradycardia during these events is more concerning than the oxygen levels as the poor heart rate means less blood is going to the brain. It is hard though to determine exactly how many events a day are actually harmful but intuitively if they are happening more than a few times a day and needing support to recover this is where we usually think about treatment.
The treatment of choice is caffeine. The same drug that is present in your soft drinks or coffee. It works by stimulating that centre in the brain that I talked about above. There are different dosing levels but you will see doses anywhere form 2.5 mg/g/d to sometimes 8 mg/kg/d for those babies with very resistant apnea. Some of those kids may need CPAP (mask on the nose) or intubation and a ventilator if they just won’t breathe. The good news is that they will grow out.
Most of our babies have their caffeine stopped sometime after they have reached the equivalent of 33 weeks (eg. born at 26 weeks this would be 7 weeks later). On rare occasion babies right up to term will have apnea as shown in the graph and for those kids if they are feeding well and otherwise ready for discharge we may choose to send you home on caffeine. Those kids though will need a follow-up study called a sleep study that will typically be done about 4 weeks later and require your child to come back for the appointment.
Blog posts of interest on apnea